Erythromelalgia
Erythromelalgia is a rare condition that causes burning pain, redness and hot skin, mainly in the feet. It can be constant or come and go, but treatment and avoiding triggers can help.
Check if it's erythromelalgia
Erythromelalgia usually affects the feet, but can also happen in the hands, arms, legs, ears and face.
The main symptoms are:
- burning pain, which often starts as itching
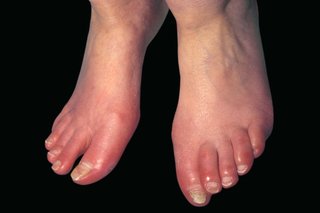
- redness – this can look different on brown or black skin
- warm or hot skin
Other symptoms include:
- swelling
- sweating more than normal
The pain can either be constant or come and go. When the pain comes, it might be called a flare-up. A flare-up can come on gradually or suddenly, and last anywhere from a few minutes to a few days.
Your skin may feel cold after a flare-up and look blue or grey.
Non-urgent advice: See a GP if:
- you have symptoms of erythromelalgia
What happens at your appointment
If a GP thinks you may have erythromelalgia, they'll refer you to a specialist.
The specialist will examine you and ask about your symptoms.
They may do tests, including blood tests and tests to look for changes in your genes that may be causing your symptoms (genetic and genomic testing).
Causes of erythromelalgia
It's often not clear what causes erythromelalgia.
Sometimes it's caused by another condition or a faulty gene inherited from one of your parents.
A flare-up of your symptoms is triggered by an increase in your body temperature.
This can be caused by:
- exercise
- wearing warm or tight clothes and shoes
- warm temperatures (such as during hot weather)
- stress
- drinking alcohol or eating spicy food
- not drinking enough fluids (dehydration)
Treatments for erythromelalgia
How erythromelalgia is treated depends on the cause.
If you have another condition that's causing your symptoms, treating that condition can help.
Most treatment aims to prevent flare-ups. It can include medicines, creams, gels, sprays, tablets and medicines given into a vein.
Rarely, you may need surgery.
Erythromelalgia can be difficult to treat. You may need to try different combinations of treatments to find the ones that work for you.
Living with pain can be difficult. If your symptoms are affecting your mental health, cognitive behavioural therapy and counselling can help.
Things that can help with erythromelalgia
There are things you can try to help control erythromelalgia symptoms and avoid flare-ups.
Do
-
try to avoid things that trigger your symptoms
-
wear loose clothing and shoes
-
drink plenty of fluids
-
try to manage stress
-
cool down your hands or feet with a fan or cool (not cold) gel pack for a short period of time
-
raise your hands or feet on a chair or pillow when you can during a flare-up
Don’t
-
do not cool down your hands or feet with cold water or use ice, as this can damage your skin
-
do not drink alcohol or eat spicy food
Page last reviewed: 18 August 2023
Next review due: 18 August 2026